Hypertonia and Hypotonia in Pediatrics
Source: surestep
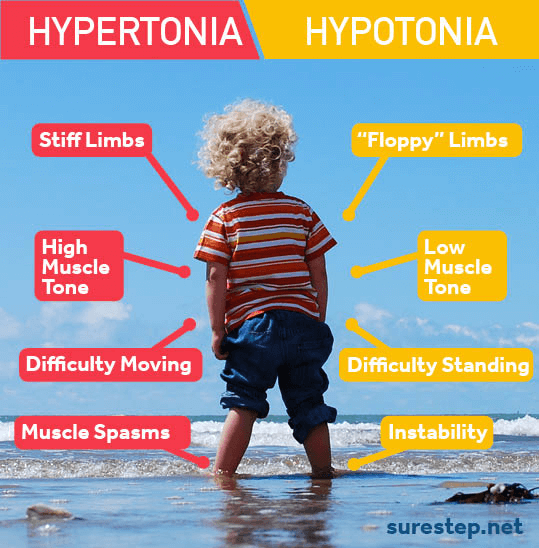
Hypertonia is a condition in which the tone of the muscle is increased, making the movement of a limb difficult. Muscle tone is regulated by the signals traveling from the brain to the nerves that signal the muscles to contract. In Hypertonia, the region of the brain that controls such signals is damaged. The main causes of Hypertonia are blow to the head, brain tumors, stroke, toxins, neurodegenerative disorders like multiple sclerosis, and neurodevelopmental abnormalities like cerebral palsy.
Causes of Hypertonia
In babies, Hypertonia is the result of an injury to the part of the brain that controls posture, movement, and reflexes. There can be many possible causes of Hypertonia including:
a. Jaundice – Jaundice, which is severe in nature and which remains untreated, can damage the brain cells of a baby resulting in Hypertonia.
b. Infection – During pregnancy, there are many types of infections like meningitis, etc., that may affect the nervous system of a fetus resulting in Hypertonia.
c. Premature birth – Babies who are born prematurely are most susceptible to cerebral palsy and can develop Hypertonia.
d. Oxygen deficiency – Severe trauma to the brain or deprivation of oxygen during labor and delivery can cause Hypertonia. When the brain doesn’t get proper oxygen and nutrients during delivery, it may cause cerebral palsy in infants.
e. Heavy metal poisoning – Ingestion of poisonous heavy metals like lead and copper is toxic to the fetus.
Symptoms of Hypertonia:
Symptoms of Hypertonia are visible once the infant is born. The most common symptoms include delayed milestones like sitting, walking, crawling, rolling, etc. Other symptoms are:
a. Spasticity (Lynn Bar-On et al., 2015).
b. Difficulty in changing positions.
c. Involuntary crossing of legs.
d. Sudden tremors during stress.
e. Loss of coordination.
f. Problem with swallowing.
g. Deformity
h. Delayed development in motor skills.
i. Problem with walking.
Hypertonia is common in cerebral palsy, but it can also affect children and infants with other pathological disorders like stroke. It’s usually difficult to move the limbs, and muscles responsible for flexion are more affected than the muscles group responsible for the extension. There may be a slight bend of the knee, and the elbow Fingers are often fisted. If Hypertonia is left untreated, then it may lead to contractures or permanent shortening of the affected muscles. The symptoms can be present in babies as small as one year and sometimes even earlier, depending upon the severity of the condition.
Physiotherapy in Hypertonic children
There are a number of treatment options in Physiotherapy to treat hypertonic children:
a. Postural management – With Hypertonia, a large number of muscles will be affected in a child, so it will affect his posture. Physiotherapy treatment to correct the posture includes relaxing the child and making it less tense so that a child can attain a natural posture.
b. Stretching – Due to the involuntary muscle contraction, a child’s limbs may not be able to move independently. Stretching can help the muscles to lengthen, and as a result, a child may be able to move his limbs more freely (Shamsoddini et al., 2014).
Source: tots2teenstherapy
c. Orthotics- Orthotics can be used along with stretching, so that right muscles are stretched for a longer duration. This can help in lengthening the affected muscles.
Source: childrenstherapyteam
d. Facilitation of normal movement – The movement of the child’s limb may be affected due to contractures and tension. Your therapist may work on the movement of your child’s limbs to achieve these activities.
e. Exercises – There are a few exercises that your physiotherapist may recommend:
i. Passive range of motion – Keep your child in a position where he can easily and comfortably move the affected body part through the available range of motion. There will be a natural stop when the limb is moved slowly. Your therapist will hold the limb at that point for a few seconds and bring it back to the starting position. As the body of your child starts to relax, there will be an increase in the range of motion.
ii. Reflex-inhibiting patterns- Reflex inhibiting patterns are the patterns that counteract the pull of spastic muscles. For example, if there is flexor spasticity, then the shoulders are elevated and internally rotated, while the elbow, wrist, and fingers are flexed. The pattern can be inhibited by gradually moving the shoulder in depression, and external rotation, while elbow, wrist, and fingers in extension. Bobath suggested the use of trunk rotation and shoulder mobilization with weight-bearing to inhibit the flexor spasticity.
iii. Weight shifting – Another way to reduce spasticity is by practicing weight shifting (Wu et al., 2017). Your therapist may recommend you gently rock your child over the therapy ball in forward and backward or side to side direction.
Hypotonia in children
Source: lookfordiagnosis
Hypotonia is a condition that is just opposite to Hypertonia. In Hypotonia, there is a decrease in muscle tone. The condition can either be due to benign congenital Hypotonia or due to other conditions in which there is progressive muscle tone loss like muscular dystrophy or cerebral palsy. Children with Hypotonia are floppy, and they exhibit ‘Rag Doll’ feelings when held. They may also fall behind in achieving motor developmental milestones and will have trouble in holding their head up, maintaining balance, getting to a sitting position, and maintaining the seated position without falling. There may also be the tendency of dislocation of the neck, jaw, and hip. In severe cases, the children may have difficulty sucking and chewing for long durations. Such children may have trouble with their speech and may exhibit shallow breathing patterns.
Causes of Hypotonia
a. Down syndrome
b. Cerebral palsy
c. Muscular dystrophy
d. Myotonic dystrophy
e. Marfan Syndrome
f. Tay-Sachs Disease
g. Prader-Will Syndrome
Symptoms of Hypotonia
Each child may show different symptoms associated with Hypotonia. Symptoms may also vary depending on the cause of the problem.
a. There will be reduced muscles tone, and muscles may feel doughy and soft.
b. The child will be able to extend the limb beyond the normal limit.
c. The child may fail to attain the motor developmental milestones like rolling over, walking sitting without support, and holding the head up without any support.
d. There may be trouble with feeding, and the child will show under active gag reflex (open mouth with tongue protruding out).
Some hypotonias have no known cause. Such a condition is known as benign congenital Hypotonia. Children having benign congenital Hypotonia have normal CNS function and intelligence. They may not have any developmental delays and can acquire gross motor skills slowly than the majority of the other children of their age.
Physiotherapy in Hypotonia
Aim of physiotherapy treatment:
a. To improve posture and core stability.
b. Strengthen the muscles around the joints for stability and support.
c. Improving body awareness and proper alignment.
To improve posture and core stability, many activities that facilitate the developmental milestones are recommended, like moving through rotational and transverse planes, shifting weight and symmetry, and pushing the surfaces using arms and feet. Sometimes a therapy ball is also used to provide challenge on the dynamic surface, which increases the vestibular input and shifting of the weight.
Source: daytonparentmagazine
When children age, the strengthening can be done through both localized and generalized activities. To improve postural control, activities are performed on dynamic and pliable surfaces. Closed chain large movements like climbing up and down to activate eccentric and concentric muscle are performed to strengthen the large muscle groups involving shoulder and pelvic girdle.
Special attention is given to improving motor control, quality of movement, and bimanual skills. Electrical stimulation (Bosques et al., 2016) can also be given to improve the strength of the muscle groups and to improve motor control. In some children, there is a need for support to improve the biomechanics and alignment. To support the imbalances, your therapist may use supportive garments to facilitate specific muscle activation. Kinesio taping (Griffin et al., 2021) can also be used. Orthotics can be very useful to improve the position of the foot. The correct movement patterns are taught to facilitate the right muscle use during movement and prevent the compensatory movement patterns.
Sensory-based techniques (Paleg et al., 2018) are taught during therapeutic activities to strengthen the muscles in Hypotonia. Joint compression and tactile input (Aman et al., 2015) are other techniques that are useful for joint support and enhancing body awareness. Your therapist may also suggest vestibular activities to improve the arousal level and increase the tone of the muscle.
No child is the same, and each child may benefit from a different type of treatment. With the right collaboration from you, your therapist may develop a treatment plan that will help in improving the condition of your child. Experts in Progressive Care will ensure that you get the best treatment for your child in a safe environment.
References:
a. Lynn Bar-On, Guy Molenaers, Erwin Aertbeliën, Anja Van Campenhout, Hilde Feys, Bart Nuttin, Kaat Desloovere, “Spasticity and Its Contribution to Hypertonia in Cerebral Palsy”, BioMed Research International, vol. 2015, Article ID 317047, 10 pages, 2015..
b. Shamsoddini, A., Amirsalari, S., Hollisaz, M. T., Rahimnia, A., & Khatibi-Aghda, A. (2014). Management of spasticity in children with cerebral palsy. Iranian Journal of pediatrics, 24(4), 345–351.
c. Wu, M., Kim, J., Arora, P., Gaebler-Spira, D. J., & Zhang, Y. (2017). Effects of the Integration of Dynamic Weight Shifting Training Into Treadmill Training on Walking Function of Children with Cerebral Palsy: A Randomized Controlled Study. American Journal of physical medicine & rehabilitation, 96(11), 765–772..
d. Bosques, G., Martin, R., McGee, L., & Sadowsky, C. (2016). Does therapeutic electrical stimulation improve function in children with disabilities? A comprehensive literature review. Journal of Pediatric Rehabilitation Medicine, 9(2), 83–99..
e. Griffin, M., McGuff, C., Willse, N., Twaddell, M., & Shin, J. (2021). Application of the Kinesio® Taping Method for a Child with Hypotonia: A Pilot Case Study. Student Journal of Occupational Therapy, 2(2), 28–41..
f. Paleg, G., Romness, M., & Livingstone, R. (2018). Interventions to improve sensory and motor outcomes for young children with central Hypotonia: A systematic review. Journal of pediatric rehabilitation medicine, 11(1), 57–70..
g. Aman, J. E., Elangovan, N., Yeh, I. L., & Konczak, J. (2015). The effectiveness of proprioceptive training for improving motor function: a systematic review. Frontiers in human neuroscience, 8, 1075.
