Osteoporosis
Osteoporosis
Osteoporosis is a term given to porous bones. It is a condition that makes your bone weak and puts you in a high-risk category for bone fractures. Many people don’t even know that they have osteoporosis unless they are diagnosed with a bone fracture.
Structure of bone in osteoporosis
Bone tissue is different than other tissues in the body. Bone tissues are hard and they keep on changing. There are two types of special cells – osteoclasts, which remove bone, and osteoblasts which form bone. Usually, there is a balance between both processes. In osteoporosis, osteoclasts remove bone at a faster rate than new bone is formed.
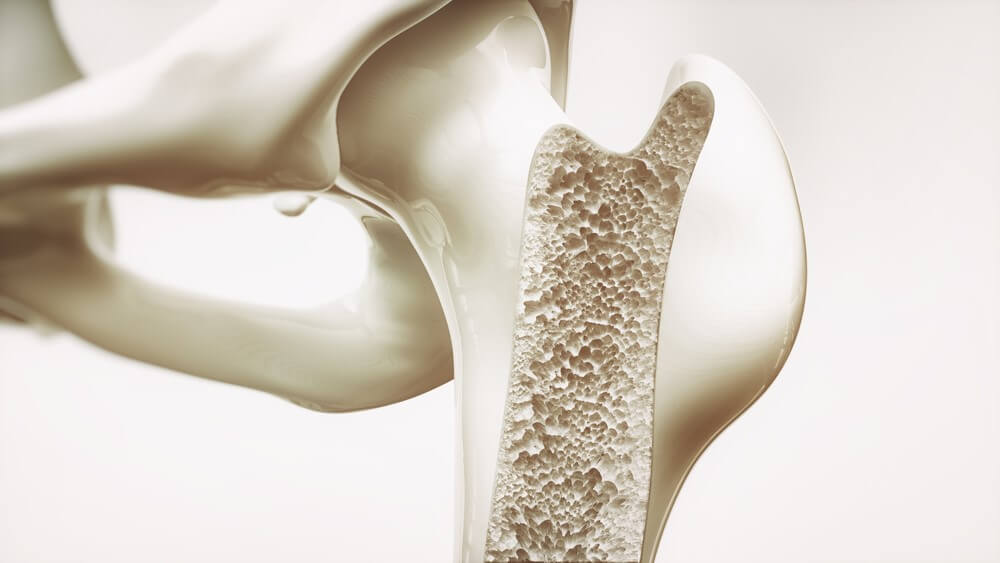
Now let’s understand the structure of the bone. There are two layers of bone – Cortical layer is the hard and outer layer, while the trabecular is a sponge-like layer and makes the internal structure of the bone. Osteoporosis causes thinning of both the cortical and trabecular bone, so your bone becomes prone to breakage.
When you see bone tissue under a microscope, you will see various honeycomb structures. In osteoporosis, the holes forming the honeycomb structure are wider and bigger. This structure of the bone is not normal and proves that you have lost the density of the bone.
Bones in osteoporosis can break much easier in the form of cracking or compression. The spine, ribs, and hips are the common bone fracture areas although fractures can occur in any skeletal bone.
Bone density and osteoporosis
Bone density is the amount of bone present in the skeletal structure. When bone density is higher, the bones are stronger. Bone density is determined by genetic factors and environmental factors. Males have higher bone density than females. Similarly, the Caucasian race has lower bone density than African Americans.
Bone density starts to accumulate in child and reach its highest at 25 years of age. It is maintained for ten years, and after the age of 35, it gradually reduces. As a part of the aging process, men and women start to lose 0.3-0.6% of bone density yearly.
Source: versusarthritis.org
Hormones play a key role in maintaining bone density. During menopause, when estrogen level takes a dip, loss of bone density speeds up. A woman may have 2-4% of bone density loss during the first 5-10 years of menopause (Finkelstein et al., 2008). This acceleration in the loss of bone density is the major cause of osteoporosis in females.
Causes of osteoporosis
Osteoporosis is caused by a decrease in bone density, so your bones get easily broken. Normally, aging causes your bone to become weaker, but in some individuals, the process happens very quickly. There are a few risk factors that make you more susceptible to developing osteoporosis. You can reduce some of the risk factors by changing your lifestyle or medication, but factors like old age cannot be changed.
Risk factors that are unchangeable:
- Age over 70 years
- Females are more prone to developing osteoporosis
- Early menopause
- Asian or Caucasian race
- Family history
- Small body frame size
Risk factors that can be changed:
- Sedentary lifestyle
- Smoking
- Low muscle mass
- Low body weight
- Excessive alcohol intake
- Not consuming enough energy-rich food
- Low calcium intake
- Eating disorders
Some diseases also increase your chance of developing osteoporosis
- Early menopause or Hypogonadism
- Diseases causing bone loss like rheumatoid arthritis
- Hyperthyroidism or hyperparathyroidism
- Kidney disease
- Chronic liver disorder
- Cushing’s syndrome
- Celiac disease
- Inflammatory bowel disease
- Cancer
Some medications can also increase your chances of being osteoporotic:
- Steroids – Steroids, when taken for a longer duration (<3 months), can make you osteoporotic (Durmaz, Berrin, 2019).
- Aromatase inhibitors – These are the drugs that block the production and working of estrogen. Aromatase inhibitors are used to prevent ovarian and breast cancer (Kilbreath, 2011).
- Antidepressants – Selective Serotonin Reuptake Inhibitor is the antidepressant that increases the level of serotonin in the brain. These drugs also increase your chance of developing osteoporotic (Rizzoli R.,2012).
- Thyroid hormone replacement therapy – If you take too much thyroid to treat your underactive thyroid, then it can also result in bone loss.
- Thiazolidinedione (TZD)- TZD is used in diabetes and is an insulin-sensitizing medication. These drugs also decrease bone formation and increase adipogenesis.
- Anti-psychotic medications – Medicines that are used in condition like Schizophrenia also causes osteoporosis.
- Anti-epileptic medications – Some anti-epileptic drugs may also increase your chance of osteoporosis.
- Proton Pump Inhibitors (PPIs) – High doses for long term of proton pump inhibitors can also increase the risk of osteoporosis (Ito, T.,& Jensen, R.T.,2010)
Complications
The main complications of osteoporosis are bone fractures, especially in the hip or spine. Hip fracture caused after a fall can result in disability and even death of the patient in the first year of the injury. Patients suffering from hip fractures will need long-term nursing care. The elderly can develop blood clots in the veins of the leg, which can travel to the lungs resulting in pulmonary embolism resulting from prolonged bed rest post-hip fracture.
Source – braceability.com
Sometimes there can be a spine fracture even if you haven’t experienced any falls. Your spine can become so weak that it can collapse, resulting in back pain, height loss, and hunched posture.
How is osteoporosis treated?
The aim of treatment is to make your bones strong so that they don’t break easily and to prevent the frequent falls by working on the balancing and strengthening of the muscles.
Drugs used for osteoporosis
Your physician may recommend medicines to make your bone strong. Some medications he may suggest are Bisphosphonates to slow down the loss of bone density and menopausal hormonal treatment to maintain the level of estrogen in menopausal women.
Diet and nutrition
Calcium – Taking proper calcium is very important to prevent osteoporosis. The best sources of calcium are dairy products like cheese, milk, yogurt, green vegetables like cabbage, broccoli, some nuts, dried fruits, etc.
Vitamin D – Vitamin D is vital for our body to absorb calcium. It is produced by the skin when your body is exposed to sunlight. Vitamin D can also be obtained from foods like oily fish. If you are someone who doesn’t go out in sunlight, then it is important that you take Vitamin D supplements.
Physiotherapy
Physiotherapy can be very beneficial in osteoporotic patients along with proper diet and lifestyle management, including quitting smoking, reducing alcohol consumption, and consuming a nutritious diet. The physiotherapy management for the individual with osteoporosis includes:
- Weight-bearing exercises – Exercises like walking have been shown to improve bone density in osteoporosis patients (Benedetti et al., 2018). The type of weight-bearing exercises depends on the overall health status of the person and how regularly that person engages in physical activity. An individual should discuss the type of exercises that he should incorporate into his daily activity with his physiotherapist. Certain movements like twisting and bending of the spine can put people at risk for fracture.
- Balance exercises – You can reduce your chances of falling by practicing the balancing exercises. Elderly people are more prone to poor balance, and studies have proved that balancing exercises can prevent falls (Hsu et al., 2014). You can start with toe and heel raises. Begin by standing while holding the high table or chair. Now slowly raise your toes and maintain the position for 10-15 seconds. Then come back to your heels. Repeat at least ten repetitions every day.
- Postural exercises – Osteoporosis may accompany structural changes such as kyphosis. Strengthening back extensors can help in improving posture and balance in individuals with osteoporosis. Extension exercises may include thoracic extensions, scapular retractions, and hip extensions. Flexion exercises are not recommended for osteoporotic patients as there can be compression fractures due to anterior compressive forces (Goodman 2003).
Regular exercises along with diet and lifestyle changes are crucial in preventing osteoporosis. With new research and medications, there will be better options for health care of osteoporotic patients in the future.
References:
- Finkelstein, J. S., Brockwell, S. E., Mehta, V., Greendale, G. A., Sowers, M. R., Ettinger, B., Lo, J. C., Johnston, J. M., Cauley, J. A., Danielson, M. E., & Neer, R. M. (2008). Bone mineral density changes during the menopause transition in a multiethnic cohort of women. The Journal of clinical endocrinology and metabolism, 93(3), 861–868.
- Durmaz, Berrin. (2019). Steroid-Induced Osteoporosis; At a Glance. American Journal of Biomedical Science & Research. 4. 147-149. 10.34297/AJBSR.2019.04.000786.
- Kilbreath, S. (2011, September). Prevention of osteoporosis as a consequence of aromatase inhibitor therapy in postmenopausal women with early breast cancer: rationale and design of a randomized controlled trial. PubMed.
- Rizzoli, R., Cooper, C., Reginster, J. Y., Abrahamsen, B., Adachi, J. D., Brandi, M. L., Bruyère, O., Compston, J., Ducy, P., Ferrari, S., Harvey, N. C., Kanis, J. A., Karsenty, G., Laslop, A., Rabenda, V., & Vestergaard, P. (2012). Antidepressant medications and osteoporosis. Bone, 51(3), 606–613.
- Ito, T., & Jensen, R. T. (2010). Association of long-term proton pump inhibitor therapy with bone fractures and effects on absorption of calcium, vitamin B12, iron, and magnesium. Current gastroenterology reports, 12(6), 448–457.
- Benedetti, M. G., Furlini, G., Zati, A., & Letizia Mauro, G. (2018). The Effectiveness of Physical Exercise on Bone Density in Osteoporotic Patients. BioMed research international, 2018, 4840531.
- Hsu, W. L., Chen, C. Y., Tsauo, J. Y., & Yang, R. S. (2014). Balance control in elderly people with osteoporosis. Journal of the Formosan Medical Association, 113(6), 334–339.
- Goodman. Fuller. Boissonnault. Pathology; Implications for the Physical Therapist. 2nd Philadelphia: Saunders, 2003.

Progressive Care Physiotherapy
Progressive Care Physiotherapy Management is the best service in the physiotherapy industry. It is known for providing the best service and cutting-edge technology to help speed up recovery, while also being able to offer various treatment options that are tailored to your specific needs.
For More details call us on 9618906780
